Sugar and Diabetes - A Complicated Relationship
Do you know what (most) peanut butter, pasta sauce, and breakfast cereals have in common? They all contain sugar! A lot, if not most, processed foods do.
Sugar consumption has increased insanely during the last couple of centuries. Two hundred years ago, Americans ate around 2 pounds of sugar per year. Today? We're at about 152 pounds per year!
What's the problem, you ask? The problem is, we've also seen an increase in metabolic conditions such as type 2 diabetes. Sugar is also nothing but empty calories. A lot of empty calories. And with a rise in obesity as well, it’s worth taking a closer look at sugar and our consumption.
Welcome to our Sugar Series, helping you understand and improve your relationship with sugar!
Before you throw out every last bit of sugar in your house, keep reading to learn about the complex relationship between sugar and diabetes.
Sugar does not trigger diabetes
Many believe sugar and diabetes go hand in hand. And while a person with diabetes will have a hard time with sugar, the relationship between the two is much more complex.
If you leave here with one thing, we hope it’s this: sugar does not trigger diabetes. Let me repeat: sugar does not trigger diabetes.
That being said, overconsumption of sugar can certainly lead to many health issues in addition to diabetic complications. And since diabetes doesn’t seem to be going anywhere anytime soon, it’s worth knowing what we’re dealing with to lower diabetes statistics.
The number of people diagnosed with diabetes, either type 1 or 2, rose from 108 million in 1980 to 422 million in 2014. And according to the CDC in the US in 2016, type 1 diabetes had a prevalence of 0.55% among adults, which is around 1.3 million, and type 2 diabetes had a prevalence of 8.6%, representing approximately 21 million adults.
The statistics for type 2 diabetes are just too high for a preventable disease.
And before we go any further into the sugar connection, we need to clarify a couple of things.
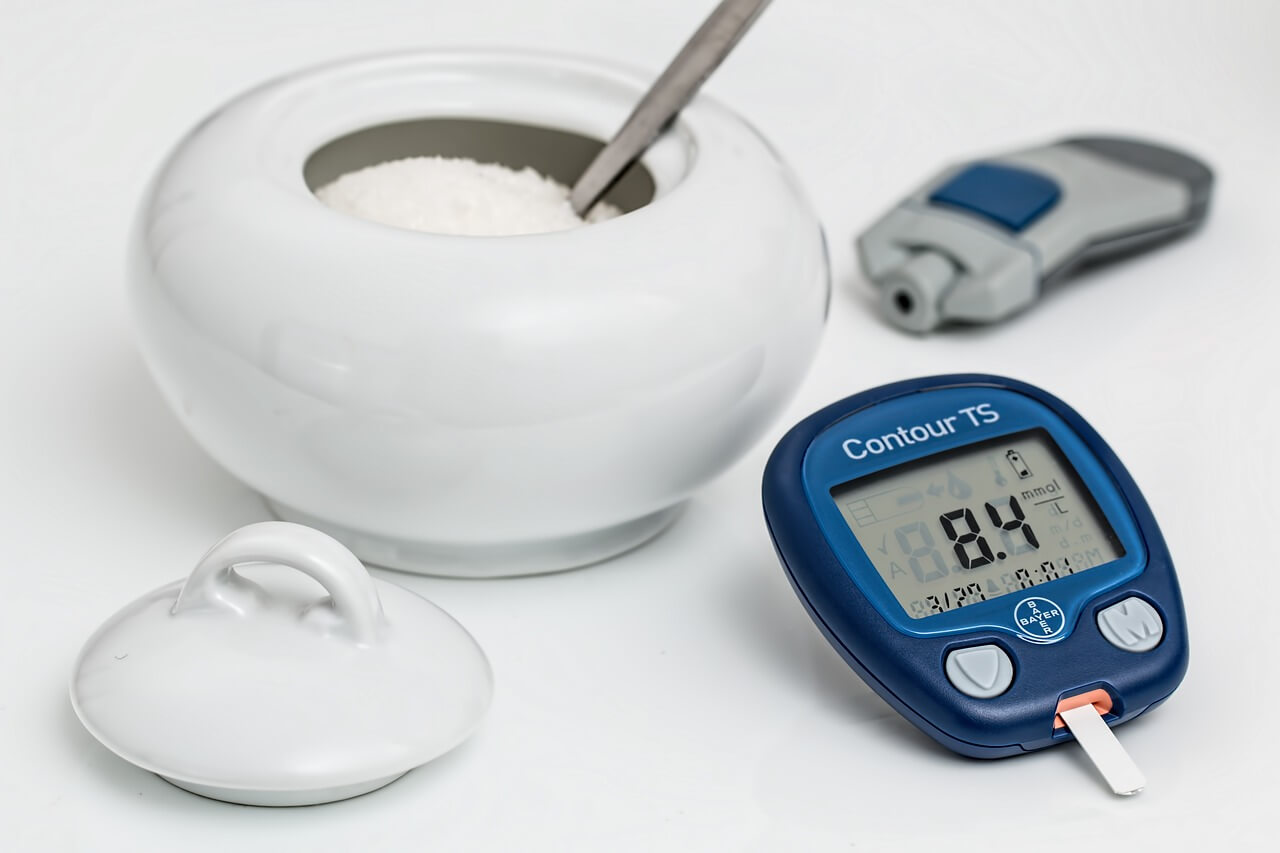
What is diabetes
First off, there are two main types of diabetes: 1 and 2. They both arise because of problems with insulin, a hormone that helps your body process sugar by getting the glucose from the bloodstream to your cells.
In type 1 diabetes, your pancreas doesn't produce insulin. This type usually starts during childhood and is dependent on insulin (often in the form of a continuous pump or self-administered injections).
In type 2 diabetes, your body produces insulin but doesn't use it properly, and usually begins in adulthood. Diet and exercise can help improve the condition by keeping blood sugar at normal levels. Sometimes, medication is required.
Type 2 diabetes is often preceded by insulin resistance. When you eat carbohydrates, your pancreas begins making insulin to help use the glucose from the carbohydrates. When your insulin sensitivity is impaired, your body responds by producing more insulin.
In time, the insulin resistance gets worse and worse until your pancreas can no longer make enough insulin. This results in high blood sugar, prediabetes, and, finally, type 2 diabetes.
We should also mention gestational diabetes, a condition that is discovered during pregnancy. And while it presents similarly to type 2 diabetes, its causes are not fully understood and it doesn’t mean you had diabetes before getting pregnant or that you’ll have it after.
Problems associated with diabetes
Diabetes, especially type 2, is a big deal because it puts you at risk for various other health conditions. But these risks can decrease if you keep the condition in check.
Heart disease and stroke are two problems commonly associated with diabetes. That's because the constant high blood sugar can lead to fatty deposits. In time, these deposits will clog your blood vessels, which in turn can lead to strokes or a heart attack. Not good.
Diabetes is also a known cause of kidney disease and kidney failure, with higher odds alongside high blood pressure and a family history of kidney disease.
Nerve damage (or neuropathy) is another risk associated with type 2 diabetes and is characterized by symptoms such as pain, numbness, or tingling in your legs. The same fatty deposits that clog your blood vessels can also impact your nerves.
The nerve damage and circulation issues can cause more damage and even lead to amputations. The nerve damage could make it hard for you to feel pain, so watch out for any sores. Unnoticed, these can become infected and eventually require amputation.

The connection with sugar
Okay, now back to the sweet stuff.
The idea that sugar causes diabetes has been discussed and examined for many years, and long story short, it’s not that simple. It takes a lot more than eating chocolate cake a few days a week to develop diabetes.
Does this mean eating sugar has no impact on your chances of getting type 2 diabetes? Not so fast. Consuming foods high in sugar will have a negative effect on your blood sugar.
It all starts with the blood sugar spike, followed by a quick drop. These constant highs and lows will eventually impact your insulin sensitivity (which can lead to prediabetes and even a type 2 diabetes diagnosis down the road).
For instance, studies have shown a 25% increase in the risk of developing diabetes in those who drink sugar-sweetened beverages regularly. And just one such drink a day is enough to increase your risk of diabetes by 13%!
Consuming added sugar on the regular may also indirectly increase your risk of diabetes. That's because, over time, it can lead to weight gain, inflammation, and increased body fat (all of which can, in turn, lead to diabetes).
Why it’s really a fat problem
While sugar plays a role in developing type 2 diabetes, it is not the only one to blame.
Recent (and even not so recent) studies show that eating fat can lead to higher blood sugar levels. Yes, you read that correctly.
Blood sugar levels may be even higher than those eating a high sugar diet, with saturated fats seemingly having the most significant impact.
The study linked above (from nearly a century ago!) found that those who ate a high-fat diet had blood sugar levels twice as high as the high-carb diet group. These surprising results can be simply explained by the fact that the fat you consume acts as a door jam preventing insulin from doing its job (pulling glucose from the bloodstream into the cell).
Coupled with the decreased insulin sensitivity mentioned earlier and the fact that high sugar foods are often high in fat, you have the perfect recipe for developing type 2 diabetes.

Fat & Sugar - Not a healthy relationship
The truth is, too much sugar or fat is bad for you. Consuming too much of both is even worse.
Another thing that is widely agreed upon is the relationship between weight and diabetes. Obesity is also on the rise and is strongly linked to type 2 diabetes.
However, remember to be mindful of fat-free food options. For instance, many fat-free dairy products are notorious for having added sugars instead. Food labels are only your friends if you read and understand the entire label.
Choosing a diet of whole foods (think fruits, vegetables, legumes, and whole grains), along with exercise and rest, is the best combination to decrease your risk of diabetes. By focusing more on whole foods, you’re automatically reducing room in your kitchen and stomach for those highly processed foods (which usually come with a lot of added sugar and saturated fat).
Other factors that may be related to the development of diabetes
Type 2 diabetes isn't all about sugar and diet in general. Other factors may increase your risk.
The first - and the hardest to fight - is genetics. If one of your parents had diabetes, you have a 40% chance of developing it. If both of your parents have/had it, your chances increase to about 70%.
Smoking is another risk factor. By smoking 20 cigarettes a day or more, you double your risk of developing diabetes. Double! The good news is that if you quit, your odds of a diabetes diagnosis go back to normal.
Another thing to consider is your activity level because a sedentary doesn’t help your odds either. A general rule of thumb is to aim for 150 minutes of moderate exercise a week.

The bottom line
The relationship between sugar and diabetes is complicated, to say the least. While eating a bit of sugar here and there won't give you diabetes, the link between the two is undeniable.
So while you don’t have to stop eating your favorite cake or candy bar, an excess of added sugar will eventually impact your insulin sensitivity, which in turn will come with many other issues. All paths can lead to diabetes.
And remember, high-fat diets aren't much better either and even contribute to the development of type 2 diabetes.
It's safe to say an excess of anything is bad. While many factors influence your chances of developing diabetes, a healthy lifestyle will undoubtedly positively impact those chances.
Now we want to hear from you! What are your biggest challenges when it comes to sugar? Did you manage to cut back on your intake? How did you do it? Follow the Silver Solution Facebook page and let us know.

Health/Medical Disclaimer
This blog post does not provide health or medical advice. This blog post is for informational and educational purposes only and is not a substitute for professional health or medical advice. Before taking any actions based upon such information, we encourage you to consult with the appropriate medical and healthcare professionals. We do not provide any kind of health or medical advice. The use or reliance of any information contained on this blog is solely at your own risk.
Sources
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4420570/
https://pubmed.ncbi.nlm.nih.gov/26199070/
https://jamanetwork.com/journals/jamainternalmedicine/article-abstract/535594
https://pubmed.ncbi.nlm.nih.gov/25599350/
https://www.cdc.gov/diabetes/data/statistics-report/diagnosed-diabetes.html
https://www.who.int/news-room/fact-sheets/detail/diabetes
Recent Posts
-
Are sunscreen ingredients harmful?
Sunny days can bring a lot of fun. Going out for a swim, spending time in nature, or relaxing on the …18th Mar 2024 -
The Veggie Debate: Does Cooking Vegetables Destroy Nutrients and the Best Ways to Cook Them
Vegetables are one of the healthiest foods you can choose. Some people downright hate them, while so …4th Mar 2024 -
Best Foods for COVID Recovery and Prevention
A few years ago, a new virus took the world by surprise. COVID-19 may look like the flu on the surfa …19th Feb 2024




